|
6/22/2023 0 Comments Mobitz type 2 On exam, she exhibited normal heart sounds without any lower extremity edema, jugular venous distention (JVD), or other signs of decompensated cardiac function. The patient’s respiratory status, however, soon worsened, and she required bilevel positive airway pressure (BiPAP). Oxygen saturation initially improved with maximum oxygen settings via nasal cannula, non-rebreather mask, and prone positioning. On admission, she was hypoxic, with an oxygen saturation via pulse oximetry of 60% on room air. Prior to presentation, she was able to freely walk several blocks but was now limited to short distances of four to eight feet uninhibited. Her shortness of breath also worsened with exertion. She described the chest pain as a dull, intermittent, and non-radiating ache. Ī 74-year-old woman with a history of diabetes presented with fever, chest pain, and shortness of breath for two days. We present the case of a patient with COVID-19 found to have profound conducting system disease resulting in a rare constellation of electrocardiographic abnormalities, namely incomplete trifascicular block and Mobitz type II atrioventricular (AV) block. Possible mechanisms of COVID-19-induced cardiac complications include hypoxia-induced myocardial injury, direct viral invasion, and inflammatory processes. A recent meta-analysis showed MERS-CoV and SARS-CoV did not cause this level of cardiac involvement, while clinical cardiac manifestations of COVID 19 are becoming apparent as the disease continues to affect patients. Moreover, in one study, 16.7% of patients experienced an arrhythmia and 7.2% experienced cardiac injury, while other studies demonstrated 23% of COVID-19 patients developed heart failure. Although the COVID-19 literature is preliminary, case reports have described myocarditis as an observed complication. In data from Wuhan, China, 19.7% of hospitalized COVID-19 patients experienced acute respiratory distress syndrome (ARDS) however, cardiac abnormalities due to COVID-19 were also found to be prevalent. As with previous iterations of coronavirus (SARS-CoV, Middle Eastern respiratory syndrome, and seasonal coronavirus), the respiratory system has been noted to be the primary target. 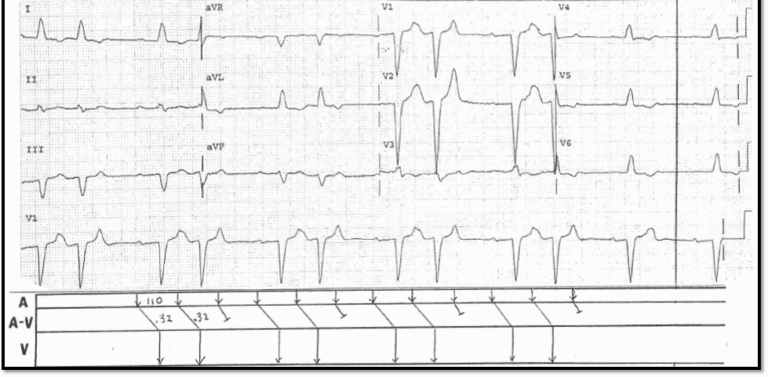
Thorough cardiac exams with electrocardiographic correlation should be performed on all patients with COVID-19. Clinicians should not hesitate to consult cardiovascular services in the event of abnormality.Ĭoronavirus disease 2019 (COVID-19), caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has affected people worldwide, with the United States having the most reported cases thus far. Further high-quality research is needed to clarify the cardiac pathophysiology. She continued to desaturate despite maximal BiPAP therapy and eventually died.Ĭardiac involvement in COVID-19, whether caused primarily by the virus, secondary to its clinical sequelae, or even due to its treatment, cannot be ignored. The patient’s oxygen requirements and mental status continued to worsen. Tocilizumab was deferred due to the patient’s age. Hydroxychloroquine was deferred due to the patient’s arrhythmia and prolonged QTc. Interleukin-6 levels were elevated at 159 pg/mL. Transcutaneous pacing pads were placed, and atropine was placed at the bedside. After noting frequent pauses on telemetry, a repeat ECG was performed that demonstrated RBBB with left posterior fascicular block as well as second-degree atrioventricular block (Mobitz type II). 
Cardiac enzymes and brain natriuretic peptide levels were within normal limits. Right bundle branch block (RBBB) with left anterior fascicular block was noted on admission electrocardiogram (ECG). Coronavirus disease 2019 (COVID-19) was confirmed. Chest X-ray demonstrated bilateral hazy opacities suspicious for viral pneumonia. 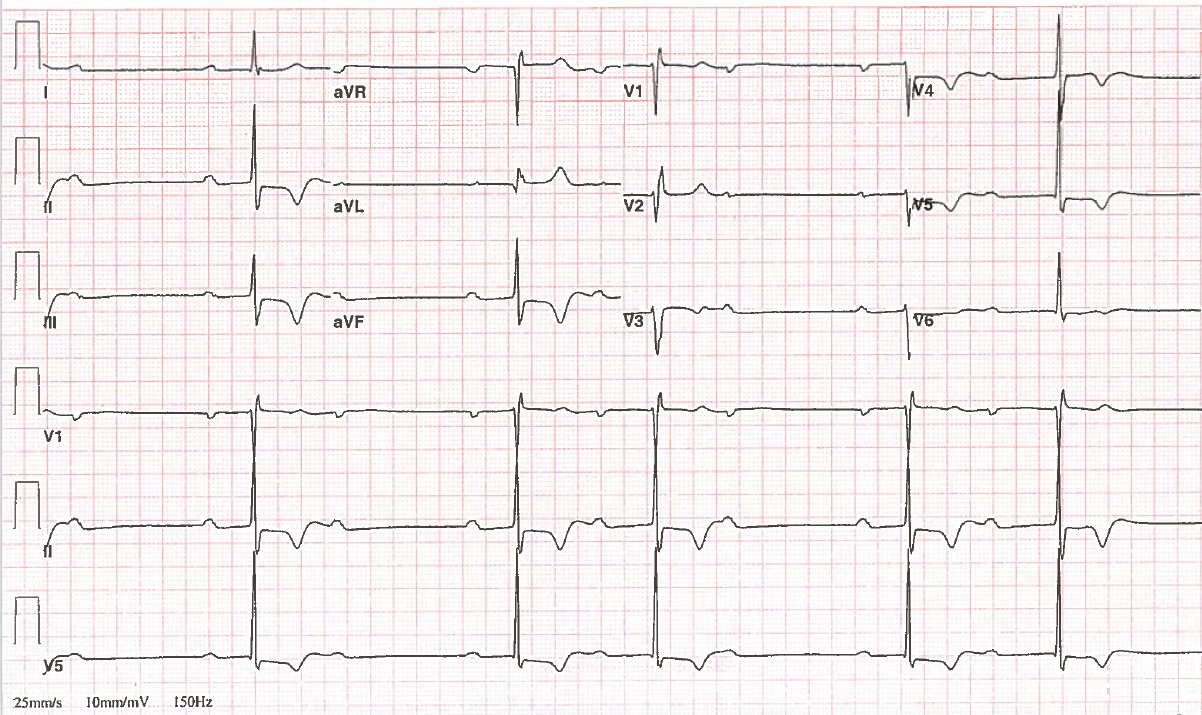
She was hypoxic to an oxygen saturation of 60% in the emergency department, requiring bilevel positive airway pressure (BiPAP) to maintain saturations. A 74-year-old female with a history of diabetes presented with chest pain and shortness of breath for two days. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
